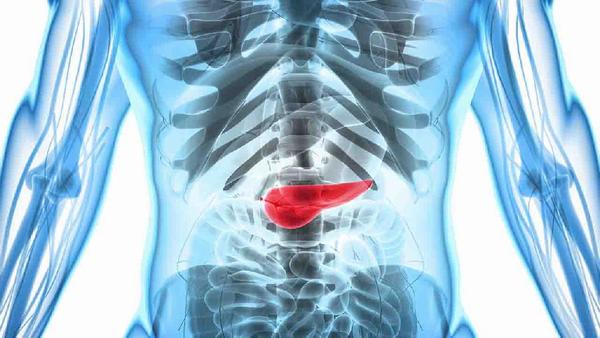
胰腺癌为什么会引起dic
 胰腺癌疾病编辑
胰腺癌疾病编辑
 胰腺癌疾病编辑
胰腺癌疾病编辑
Title: The Connection between Pancreatic Cancer and DIC: Unraveling the Enigma
Introduction:

Pancreatic cancer, a highly aggressive and deadly form of cancer, is notorious for its poor prognosis. Apart from its devastating impact on the affected individuals, pancreatic cancer often presents with several associated complications, including Disseminated Intravascular Coagulation (DIC). DIC is a serious condition characterized by widespread clotting throughout the bloodstream, leading to severe bleeding and organ dysfunction. In this article, we will explore the intricate relationship between pancreatic cancer and DIC, shedding light on why this malignancy increases the risk of DIC development.
Understanding Pancreatic Cancer:
Pancreatic cancer originates in the tissues of the pancreas, an organ located behind the stomach. It is characterized by the uncontrolled growth of abnormal cells in the pancreas, which ultimately form tumors. Unfortunately, pancreatic cancer is often diagnosed at advanced stages, when it has already spread to nearby organs, making it difficult to treat effectively.
The Link to DIC:
DIC is a condition in which the body's normal blood clotting mechanisms become dysregulated, resulting in excessive clot formation simultaneously with increased bleeding tendencies. While DIC can be triggered by various factors, it is frequently observed in individuals with pancreatic cancer. Several mechanisms contribute to the development of DIC in pancreatic cancer patients:
1. Overproduction of Tissue Factor:
Pancreatic cancer cells release substances known as tissue factors, which initiate blood clot formation. The increased production and release of tissue factor by cancer cells in the pancreas can trigger the initiation of coagulation pathways, leading to DIC.
2. Abnormal Activation of the Coagulation System:
In pancreatic cancer, the balance between procoagulant and anticoagulant factors in the bloodstream becomes disrupted. Cancer-associated inflammation and the presence of tumor-derived procoagulant substances promote the activation of the coagulation system, favoring clot formation.
3. Involvement of Platelets:
Platelets play a crucial role in the formation of blood clots. In pancreatic cancer, platelets become activated and aggregate around the tumor site, contributing to the formation of microclots. This platelet adhesion and aggregation further exacerbate the risk of DIC development.
4. Impaired Fibrinolysis:
Fibrinolysis is the process by which the body breaks down blood clots. In pancreatic cancer, the balance between clot formation and clot breakdown is disrupted. Cancer cells release substances that inhibit the activity of fibrinolysis, leading to the persistence of clots within blood vessels.
Clinical Manifestations and Management:
DIC resulting from pancreatic cancer presents with symptoms such as abnormal bleeding, easy bruising, organ dysfunction, and thromboembolic complications. When DIC occurs, it further hampers the prognosis of pancreatic cancer patients, increasing the risk of complications and mortality.
Management of DIC in pancreatic cancer involves addressing the underlying cancer itself. Treatment strategies may include surgical resection of the tumor, chemotherapy, radiation therapy, and palliative care to alleviate symptoms. DIC-specific management includes the administration of blood products, anticoagulants, and supportive measures to stabilize the patient's condition.
Conclusion:
The connection between pancreatic cancer and DIC is a complex interaction of various factors, including abnormal coagulation, platelet activation, and impaired fibrinolysis. These mechanisms contribute to the development of DIC in pancreatic cancer patients and further complicate their prognosis and treatment options. Understanding the intricacies of this relationship is crucial for developing targeted therapeutic interventions and improving the outcomes of individuals affected by both pancreatic cancer and DIC.